Diabetes and cataract often go hand in hand. Diabetes is a condition that acts as a troublemaker in the body, particularly when it involves insulin – that crucial hormone responsible for shuttling sugar into your cells. When this system is off-kilter, you could end up with an excess of glucose in your bloodstream, leading to elevated blood sugar levels.
Now, high blood sugar can be a real party crasher, leading to a whole array of health issues ranging from nerve damage to heart problems. Yet, that’s not the end of the story. There’s another guest on the list of potential complications: cataracts.
For those who might not be familiar, a cataract is basically when the lens of your eye decides to go rogue and become cloudy, leaving you with vision that’s about as clear as looking through a steamy window. It’s not exactly a pleasant experience, and it’s a condition that seems to buddy up with diabetes more often than we’d like.
The folks over at the Centers for Disease Control and Prevention (CDC) have crunched the numbers, and it turns out that around 32.2 percent of adults over the age of 45 who are living with diabetes also have cataracts. That’s a significant chunk, and it highlights just how interconnected these two conditions are.

Understanding the Relationship: Diabetes and Cataracts
When we talk about diabetes and cataracts, blood sugar is the main character in our story. Now, let’s dive a bit deeper to truly grasp how these two are linked and why managing blood sugar is so crucial.
High blood sugar, if it becomes a regular visitor, can start causing trouble in various parts of your body, including those tiny blood vessels in your eyes. It’s like a domino effect; once diabetes starts to influence these vessels, the risk of cataracts and other eye conditions climbs up the chart.
So, here’s the deal with cataracts: they form when sugar levels decide to throw a party in the aqueous humor. And no, we’re not talking about a sense of humor here. The aqueous humor is the space hanging out between your eyeballs and the lens of your cornea, playing the vital role of supplying nutrients and oxygen to the lens.
When the blood sugar decides to spike, it’s like blowing up a balloon in your lens, causing it to swell and your vision to blur. But wait, there’s more. Unchecked blood sugar has a trick up its sleeve, transforming glucose with the help of enzymes in the lens into a substance known as sorbitol. And just like having too many cooks in the kitchen, too much sorbitol in your lens leads to cloudy vision.
Navigating Through Cataract Surgery and What Comes After
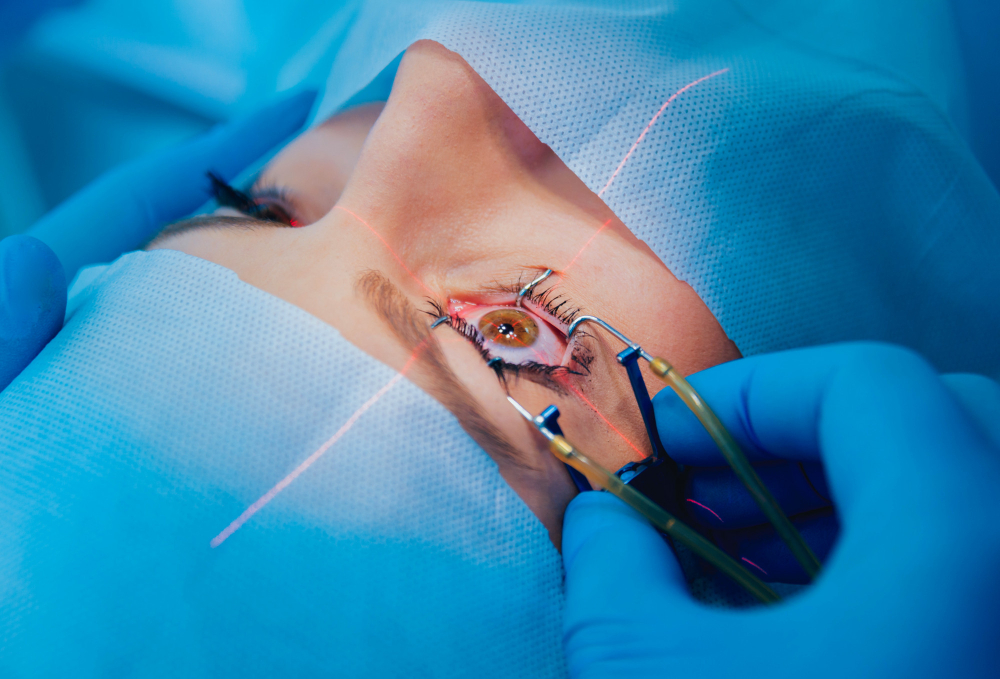
Cataract surgery stands as a beacon of hope for those grappling with the cloudy vision caused by diabetes-induced cataracts. It’s a straightforward outpatient adventure where your surgeon swaps out the faulty lens with a shiny new artificial one.
Deciding on the Right Time for Surgery
Not every cataract demands immediate surgery. For the milder cases, a simple tweak in your eyeglasses prescription might just do the trick to clear up that blur. However, when a cataract throws a tantrum and gets worse, it starts meddling with your daily life—making driving, reading, and even navigating stairs feel like a Herculean task.
Here’s How the Magic Happens
The goal of cataract surgery? Crystal clear vision. And the good news? It’s usually a quick in-and-out procedure, wrapping up in about 30 minutes to an hour.
First, your eye surgeon will drop some dilation magic in your eye, giving them a clear view inside. Then comes the local anesthesia to numb the area, and perhaps a sedative to kick back and relax—you’ll be awake but won’t feel a thing.
To evict the cataract, a small cut is made in the cornea, followed by an ultrasound probe that breaks up and vacuums out the unwelcome guest. Post-cataract eviction, in goes the new artificial lens, a few stitches to the cornea, and voila!
The Road to Recovery
Don’t expect superhero vision right off the bat. It’s more of a slow burn, with your eyesight gradually sharpening over a few days. You’ll be rocking an eyepatch for a bit and armed with prescription eyedrops to fend off inflammation and infections.
Cataract surgery boasts an impressive success track record, and once that cataract is gone, it’s gone for good. But, a word to the wise: keeping that blood sugar in check is key to preventing future cataracts from crashing the party.
Special Considerations for the Diabetes Crew
Now, if you’re part of the diabetes club, your post-surgery experience might have a few extra twists and turns, especially if you’ve got other eye conditions like glaucoma or diabetic retinopathy in the mix. In these cases, you might still have a bit of blur lingering post-surgery.
And don’t forget: having your blood sugar levels on your side before diving into surgery is crucial. High blood sugar can throw a wrench in the healing process and crank up the risks of infections and bleeding.
Guarding Your Eyes: A Guide to Cataract Prevention for Diabetes Warriors
Living with diabetes? Don’t worry, you’ve got this—and when it comes to staving off cataracts, maintaining a steady blood sugar level is your secret weapon. Here’s your game plan: keep a watchful eye on that blood sugar and stick to your diabetes meds like glue.
Hit a snag and your blood sugar’s still doing the cha-cha on the high side? Don’t wait it out—get on the horn with a healthcare pro who can tweak your meds and get things back on track.
Now, let’s talk about flexing those muscles. Regular exercise is like a secret potion for blood sugar control. It gets your muscles grooving and using glucose the right way, and can even throw a wrench in type 2 diabetes’ sneaky plans to progress.
Ready to get moving? Here are some blood-sugar-busting activities to add to your playlist:
- Speedy walking
- Biking
- Exploring trails
- Dancing like nobody’s watching
- Taking a dip in the pool
- Getting competitive in sports
But wait, there’s more! Don’t forget to pencil in a date with your eye doctor at least once a year for a comprehensive eye exam. Keep your blood pressure and cholesterol in the sweet spot, and if tobacco’s in the picture, it’s time to say “it’s not me, it’s you.”
This piece is tailored to maintain a semi-formal yet engaging tone, ensuring the reader feels empowered and informed on their journey to preventing cataracts with diabetes. Adjustments can
Wrapping It Up: The Final Take on Cataracts and Diabetes
So, here’s the deal: cataracts don’t play favorites—they can show up in just about anyone’s life, but they do seem to have a bit of a soft spot for folks dealing with diabetes. The silver lining? Cataract surgery is a game-changer, and it’s got a pretty stellar track record for bringing clear vision back to the table.
But remember, it’s not a one-size-fits-all situation. While a lot of people walk away from surgery seeing the world in high definition, the level of clarity you get to enjoy is really dependent on the overall wellbeing of your peepers and whether you’re juggling any other diabetes-related eye conditions.
This conclusion maintains a friendly, conversational tone while summing up the key points of the article, ensuring the reader leaves feeling informed and hopeful. Adjust as necessary to suit your style or to seamlessly integrate with the rest of your content!
References
- Cataracts. (n.d.).
https://www.aoa.org/healthy-eyes/eye-and-vision-conditions/cataract?sso=y - Diabetes and cataracts. (2019).
https://www.diabetes.co.uk/diabetes-complications/cataracts.html - Eye disorders and vision loss among U.S. adults aged 45 and over with diagnosed diabetes, 2016–2017. (2019).
https://www.cdc.gov/nchs/products/databriefs/db344.htm - Manage blood sugar. (2020).
https://www.cdc.gov/diabetes/managing/manage-blood-sugar.html - Management of diabetes before and after surgery or procedure. (n.d.).
https://www.wsh.nhs.uk/CMS-Documents/Patient-leaflets/DiabetesUnit/5830-3-Diabetes-Management-of-diabetes-before-and-after-surgery-or-procedure.pdf