Cataract Surgery Complications are rare, but it’s crucial to understand that while cataract surgery is typically a straightforward process yielding enhanced vision and minimal long-term issues, there are certain risks involved. These risks can include eye problems or the impact of pre-existing medical conditions.
Knowing about potential complications is essential for informed decision-making. After your surgery, remain vigilant for any unusual symptoms and promptly consult your doctor if you notice anything concerning.
Is a Do-Over Possible with Cataract Surgery?
Cataract surgery often brings remarkable improvements to one’s quality of life. Yet, like any medical procedure, it’s not without its risks of unwanted outcomes.
Your eye surgeon will discuss the risks before surgery. In cases where the surgery doesn’t meet expectations, there are additional treatments available to achieve a satisfactory result.
Key Risks of Cataract Surgery Complications to Keep in Mind
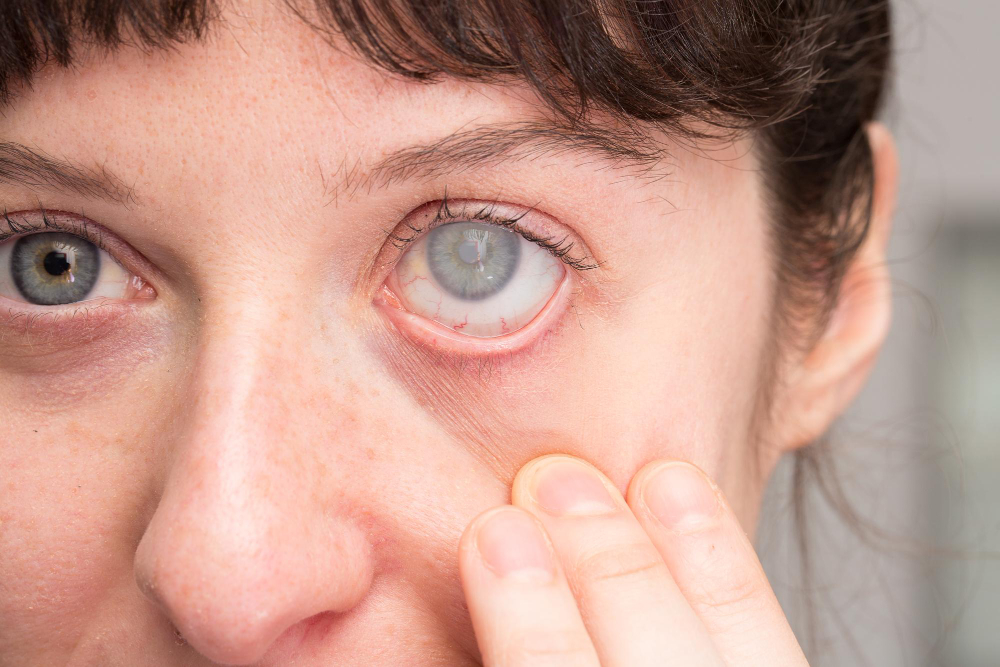
While cataract surgery has an impressive 98% success rate, understanding Cataract Surgery Complications is essential as all surgeries carry risks. Potential issues, though rare, can range from minor discomfort to more severe problems like vision loss or, in extreme cases, the necessity for eye removal.
These complications can include infection, detached retina, inflammation, swelling, remnants of the cataract, glaucoma, bleeding, and worsening of existing eye conditions such as diabetic retinopathy. Additionally, if other eye diseases like macular degeneration are present, there might be inadequate vision improvement, potentially requiring further treatment or additional surgery.
Post-Surgery Infection: A Rare But Serious Concern
Infection can occur if bacteria enter the eye during surgery, leading to symptoms like light sensitivity, pain, redness, and vision disturbances. Immediate medical attention is crucial in these cases.
Although rare, treatment for post-surgical infection typically involves an antibiotic injection in the eye, and sometimes, removal of the vitreous to prevent the infection from spreading.
Managing Inflammation After Cataract Surgery
Experiencing mild swelling and redness post-surgery is normal. If these symptoms intensify, your doctor may prescribe eye drops or other medications to mitigate them effectively.
Addressing Retinal Fluid Buildup After Cataract Surgery
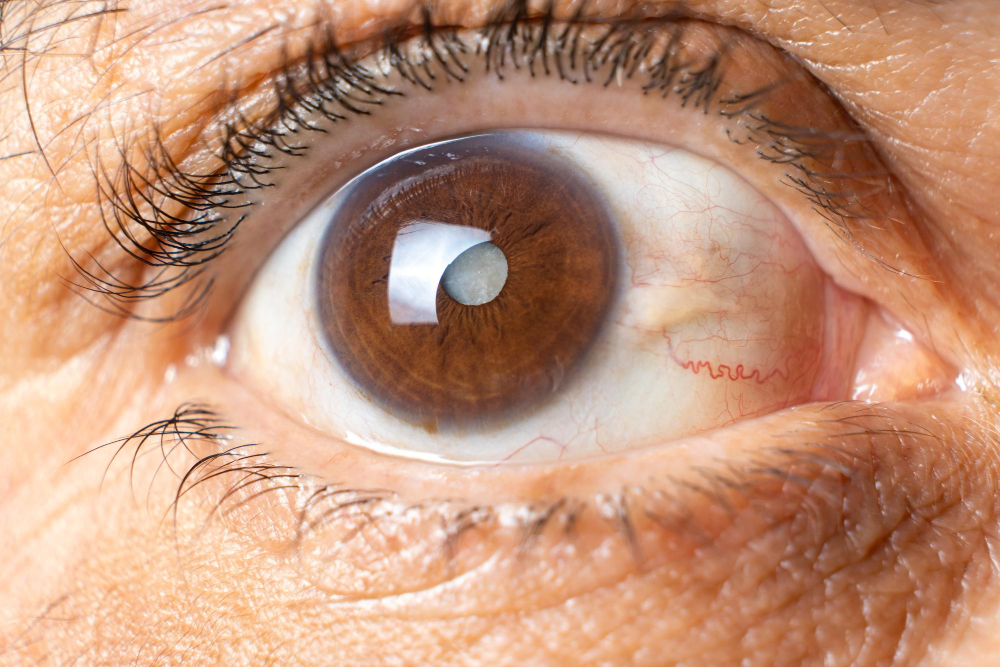
A common concern post-cataract surgery is fluid accumulation in the retina, a condition triggered by leaking blood vessels. This can blur vision temporarily. Typically, your doctor will prescribe eye drops to remedy this, which might take several weeks, sometimes months, to show full effect. While this condition usually resolves on its own, more serious instances might necessitate a steroid injection or even surgery behind the eye for complete resolution.
Navigating the Challenge of a Dislocated Intraocular Lens (IOL)
One possible complication during cataract surgery is the misplacement of the Intraocular Lens (IOL). If the artificial lens implant isn’t correctly positioned, it can lead to blurred or double vision. In some instances, the IOL may be manually repositioned by your surgeon. However, if repositioning isn’t feasible, additional surgery might be required, potentially involving the replacement of the IOL.
Understanding and Treating Secondary Cataract (Posterior Capsule Opacification)
Posterior capsule opacification (PCO), a common Cataract Surgery Complication often referred to as secondary cataract, is a phenomenon that may occur after the procedure. During cataract surgery, the lens’s front part is removed while the enclosing capsule is left intact. Over time, this can result in haziness in vision, mirroring the symptoms of the original cataract.
The standard treatment for PCO, a typical Cataract Surgery Complication, is a procedure known as YAG laser capsulotomy. This efficient and painless procedure uses a laser to create a small opening in the back of the lens capsule, enabling light to pass through and restore clear vision. Taking just about five minutes, YAG laser capsulotomy is a routine follow-up for many patients post-cataract surgery and is an expected part of the recovery process.
Managing Corneal Swelling Post-Surgery
The cornea, the eye’s clear front layer, may swell after cataract surgery, causing temporary blurring of vision. This swelling usually subsides within a few days to weeks. Treatment generally includes the use of prescribed eye drops to reduce inflammation and speed up the healing process.
Dealing with Bleeding Post-Cataract Surgery
A common postoperative experience, often categorized under Cataract Surgery Complications, is the perception of floaters and flashes of light. This occurs when the vitreous, the gel-like substance inside the eye, separates from the retina. Patients undergoing cataract surgery often describe seeing moving web-like patterns, cloudy spots, and sudden flashes of light. While these symptoms can be alarming, mirroring those of retinal detachment, they usually necessitate a prompt evaluation by your doctor. However, in most cases, these symptoms associated with Cataract Surgery Complications gradually resolve within a few months as the eye heals
Managing Increased Eye Pressure After Surgery

Ocular hypertension, or increased pressure within the eye, is another potential aftermath of cataract surgery. This condition can impact vision and requires careful management. Treatment typically involves the use of prescribed medications such as eye drops, oral medications, or injections.
In some cases, this increased pressure can lead to glaucoma, particularly if it’s caused by factors like swelling, bleeding, or residual lens fragments. The treatment strategy for glaucoma will depend on the underlying cause and may range from medication to more advanced interventions like glaucoma surgery, especially if there is damage to the optic nerve.
Dealing with Post-Surgical Light Sensitivity
It’s not unusual to experience increased sensitivity to light following cataract surgery. While this usually subsides within a couple of days, prolonged sensitivity might indicate other underlying issues such as excessive inflammation, requiring medical attention and potentially the use of anti-inflammatory eye drops. Patients are often advised to wear sunglasses for a few months post-surgery to alleviate discomfort.
Addressing Droopy Eyelid (Ptosis) Complications
Ptosis, or drooping of the eyelid, is a relatively common occurrence after cataract surgery. The exact cause of this condition is often unclear, and it typically resolves without any intervention. However, if ptosis persists for more than six months, surgical correction might become necessary to restore normal eyelid function and appearance.
Dysphotopsia: Unusual Visual Effects

Dysphotopsia refers to unusual visual effects experienced post-surgery. There are two main types:
- Negative Dysphotopsia: This manifests as a dark, curved shadow at the edge of your vision. While its cause is still debated among experts, this type of dysphotopsia often diminishes over time. However, it can sometimes persist longer than its counterpart.
- Positive Dysphotopsia: This type leads to visual disturbances like halos, starbursts, or streaks of light. It is generally temporary and tends to resolve on its own.
The typical approach to managing dysphotopsia involves watchful waiting to see if the condition improves over time. In some cases, eye drops or glasses with heavier frames can help reduce the severity of the shadows. If dysphotopsia continues for an extended period, your doctor may consider other interventions, such as replacing the lens or using a combination of lenses to alleviate symptoms.
Understanding the Possibility of Cataract Recurrence Post-Surgery
A common question that arises after cataract surgery is whether cataracts can recur. It’s important to clarify that once cataracts are removed, they cannot return. This is because the surgery involves the removal of the natural lens, where the cataract forms. However, a condition often mistaken for cataract recurrence does exist, known as Posterior Capsular Opacity (PCO).
Posterior Capsular Opacity: A Look-Alike Condition
While cataracts themselves don’t recur, PCO can develop, giving rise to symptoms similar to those of cataracts, such as haziness or clouding of vision. This condition occurs when the back portion of the lens capsule, which is left intact during cataract surgery to support the lens implant, becomes opaque over time.
PCO is sometimes informally referred to as a “secondary cataract,” but it’s crucial to understand that it’s not a true cataract. Instead, it’s a cell growth on the residual lens capsule, which can hinder clear vision by scattering or blocking light as it passes through the lens of the eye.
Diagnosis and Treatment of Posterior Capsular Opacity
The diagnosis of PCO is typically made during a routine eye examination. Symptoms can appear months or even years after the initial cataract surgery. When PCO is identified, the standard treatment is a YAG laser capsulotomy. This simple, painless procedure involves using a laser to create a small opening in the cloudy capsule, allowing light to pass through clearly again. The procedure is quick, typically taking only a few minutes, and is highly effective at restoring clear vision.
Preventive Measures and Long-Term Care
While it’s not always possible to prevent PCO, regular eye exams post-cataract surgery can help in early detection and treatment. It’s also important for patients to maintain good eye health practices, such as protecting their eyes from excessive UV light and managing underlying health conditions that could affect their eyes.
In conclusion, while cataracts themselves do not recur after surgery, the development of PCO is a possibility. However, with modern treatment methods, this condition can be effectively managed, ensuring that patients continue to enjoy clear vision long after their cataract surgery.